One of the most impactful dementia training sessions I have participated in over the last 20+ years focused on Maslow’s Hierarchy of Needs and serving senior adults with Alzheimer’s or other dementia. To be honest, I wasn’t excited about going as Maslow brought back junior high memories of attending class, taking tests, and doing homework! I’m so glad I didn’t let that keep me from attending. And to be clear, I’m not a psychologist nor have I studied much psychology, but I’ve seen people with dementia having needs met and unmet and how that affected their behavior.
A Brief Background on Maslow
Abraham Maslow was an American psychologist (1908-1970) who published a 1943 paper entitled “A Theory of Human Motivation” in Psychological Review. This paper proposed Maslow’s hierarchy of needs, an idea of psychology with little scientific basis. Even so, a 2002 survey conducted by Review of General Psychology ranked Maslow as the 10th most cited psychologist of the 20th century. Needless to say, very few students could get through high school having never heard about this hierarchy of needs.
Maslow’s Hierarchy of Needs
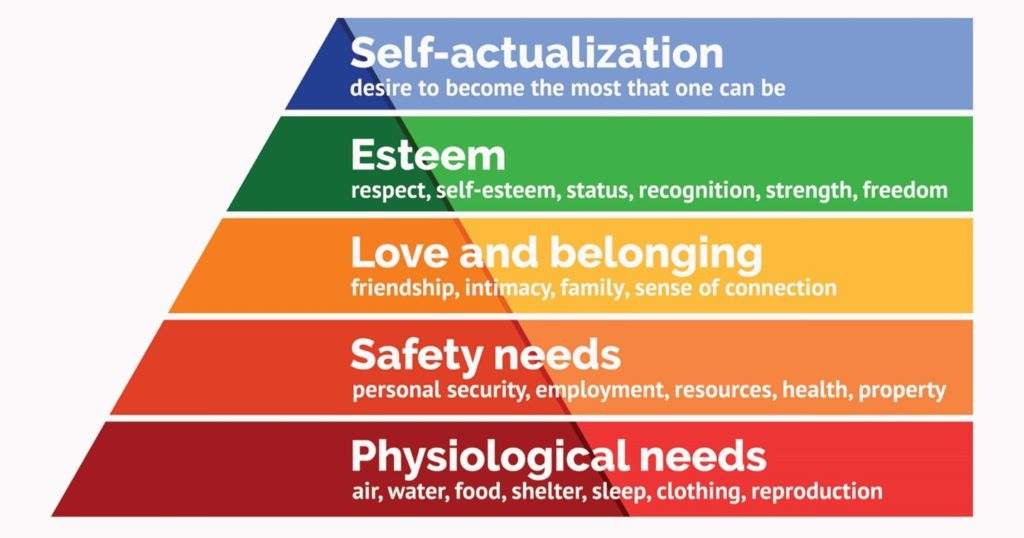
So, the general idea is that we all move “up the triangle” as our needs are met, from the very basic needs of food and shelter to realizing one’s full potential. While I understand there are those that agree and disagree with how one may flow up and down through the hierarchy, let’s apply this model to someone living with a diagnosis of dementia.
Getting “To the Top” of the Triangle
Each day in the life of a person with dementia can be a brand-new adventure. Many caregivers work very hard to establish routine and familiarity as they carefully meet the needs of their loved one, setting them up for success. Consider the following “needs” as they relate to Maslow:
- Physiological Needs
- Has your loved one forgotten to eat or drink?
- Does he/she know how to tell you when they’re hungry or thirsty?
- What about the ability to communicate that he/she needs to go to the bathroom?
- With sleep patterns often being affected, can your loved one carry out the most basic functions?
PRACTICAL TIPS
-
-
- Prepare meals that are easy to eat (e.g. finger foods)
- Frequently offer water to stay hydrated
- Implement a bathroom schedule
- Stay active during the day to help with sleeping at night
-
- Safety Needs
- Does your loved one feel like they’re in a strange place – do they realize they are at home or has something changed that makes them experience fear or anxiety?
- The person with dementia may think that they can’t afford a meal, or he/she doesn’t understand how things are being paid for (rent, mortgage, transportation, etc.).
PRACTICAL TIPS
-
-
- Maintain a familiar environment – pictures of family, favorite chair and blanket
- Assure your loved one that expenses are taken care of (e.g. “Oh, yes, you paid that bill last week” or “your friend, Martha, wanted to treat you to lunch today)
-
- Love and Belonging
- Many elderly people with dementia have lost loved ones over the years. They may ask for a parent or spouse, people with whom they’ve had long-term, close relationships. They long for that sense of belonging and intimacy.
PRACTICAL TIPS
-
-
- Validate or Redirect when asked about deceased loved ones (never put them through grief again by telling them the person has died)
- As a caregiver, your demeanor of love and compassion will help the person with dementia to feel as though they belong and are loved
-
- Esteem
- The feeling of being respected and maintaining dignity don’t go away with the disease
- No one wants to feel inferior or incapable
PRACTICAL TIPS
-
-
- Validate the person’s thoughts and actions
- Do not correct them; instead, redirect kindly
- Engage in activities that your loved one can master
- Ask simple questions and communicate clearly
-
- Self-Actualization
- With the other sets of needs being met, your loved one will likely feel content, social, glad to see you, etc. – kind of like we all do when our basic needs are met, we are safe and secure, we feel loved and that we belong, and finally, that we feel capable and equal with others.
Maintaining a level at or near the top of Maslow’s triangle isn’t easy, nor is it going to happen every day. Doing what you can to stay engaged and aware is important – this will lessen the chance of falling back down the triangle. Validating one’s feelings and thoughts should be a recurring theme throughout the day. The time for arguing or trying to rationalize is likely passed.
It can quickly become overwhelming to think about all the needs that must be tended to in a day for a person with dementia. There are no two cases just alike and there is no one magic answer. At Covenant Caregivers, we would strongly recommend finding ways to get a break, whether through family members pitching in or hiring a professional caregiver. For a free consultation, give us a call at 601-856-5660.